What is Atrial Tachycardia?
Atrial tachycardia (AT) is a type of heart arrhythmia that causes your heart to beat 100 to 300 times each minute. A normal heart rate at rest is 60 to 80 beats each minute. AT develops because of problems with your heart's electrical system. Your atria (top chambers) may send electrical signals that increase your heart rate, or the pathway of the electrical signal may be blocked. Your heart keeps sending signals to try to get past the block.
Atrial Tachycardia vs. Atrial Fibrillation
Atrial tachycardia and atrial fibrillation are very similar. They both affect the atria of the heart. The difference between the two is the regularity of the heart rate. In tachycardia, the heart rate is fast, over 100 beats per minute, but is regular. In fibrillation, the electrical signals fire in a very fast or uncontrolled manner, causing the atrial chambers of the heart to twitch, quiver, flutter, or contract.
What causes Atrial Tachycardia?
Atrial tachycardia usually occurs in elderly patients and in those who already have other types of heart disease. It also occurs in children who have problems such as congenital heart disease. When the patient has a heart rate over 100 beats per minute, it is called tachycardia. These are the typical causes:
- A previous heart attack
- A “stretched” atrium due to high blood pressure or cardiomyopathy

- Consuming too much caffeine
- Use of cocaine or methamphetamines
- Excessive alcohol use
- Chronic lung disease
- Pregnancy
- Certain medications, such as asthma and allergy drugs
Atrial Tachycardia Symptoms
You may feel any of the following:
- Lightheaded, dizzy, or faint
- Jumping or fluttering in your chest
- More tired than usual
- New or increased shortness of breath
- Pain, pressure, or tightness in your chest
- The need to urinate more often than usual
Atrial Tachycardia Diagnosis
Dr. Smith can diagnose atrial tachycardia in his office with an electrocardiogram (ECG/EKG), but when the elevated heart rates are only occasional occurrences, the ECG may show “normal” results. In these cases, Dr. Smith will have you wear an ECG monitor at home. This will record your heart rhythm over time. These monitors include:
- Holter monitor — A portable ECG you wear as you go about your routine.
- Event monitor — A portable ECG you wear for one or two months. It only begins recording when triggered by an abnormal heart rhythm or when you manually activate it.
- Implantable monitor — A tiny event monitor can be implanted under your skin. It is worn for several days to record events when they only occur occasionally.
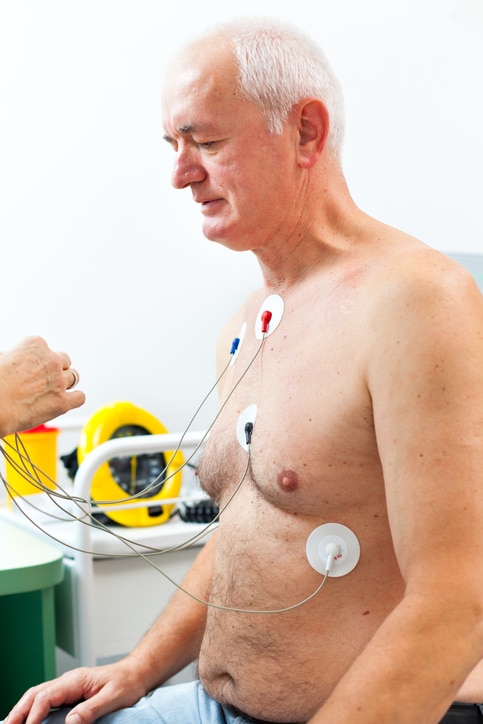
Blood tests can be used to check thyroid function, heart disease, and other conditions that can trigger atrial tachycardia. Stress tests done on a treadmill or stationary bike can also be used to monitor heart activity.
What kind of Atrial Tachycardia treatment is right for me?
Depending on your diagnosis, Dr. Smith has various treatment options. These include:
- Medications — Medications can control your heart rhythm. These include beta-blockers, calcium channel blockers, and antiarrhythmic medications.
- Cardioversion — In cardioversion, Dr. Smith delivers a shock to your heart through paddles or patches placed on the chest. The current affects the heart’s electrical impulses and can restore a normal rhythm.
- Catheter ablation — A catheter is threaded through a blood vessel to the heart. An electrode at the tip of the catheter delivers either heat, extreme cold, or radiofrequency energy to damage (ablate) a small spot of heart tissue. This stops that area from sending the incorrect electrical messages that are causing the tachycardia.
How can I prevent Atrial Tachycardia?
Much of the regimen to keep your heart healthy applies here.
- Eat a diet with whole grains, fruits, vegetables, and lean protein. If you’re overweight, this adds stress to your heart, which can help trigger tachycardia. Try and eat more foods with potassium and magnesium in them.
- Cut down on foods that can trigger a faster heartbeat: alcohol, caffeine, spicy foods, and even very cold drinks.
- Hard exercise can trigger a bout of atrial tachycardia, but exercise is still important. Dr. Smith will discuss exercises that will work for your situation.
- Lower your stress levels.
What happens if I don’t treat my Atrial Tachycardia?
Without treatment, your symptoms may get worse. Your heart may not be able to pump enough blood to supply oxygen to the rest of your body. You may get a blood clot. The clot can break loose and travel to your lungs or brain. A blood clot can cause you to have a stroke. Your heart may weaken and not work properly. You are also at a higher risk for a heart attack and heart failure.
Schedule a Consultation
If you are suffering from atrial tachycardia, you should learn more about your treatment options. Call 205-971-7566 to schedule a consultation with Dr. Macy C. Smith. Dr. Smith serves Birmingham, Alabama and surrounding areas.