What is Atrial Fibrillation (AFib)?
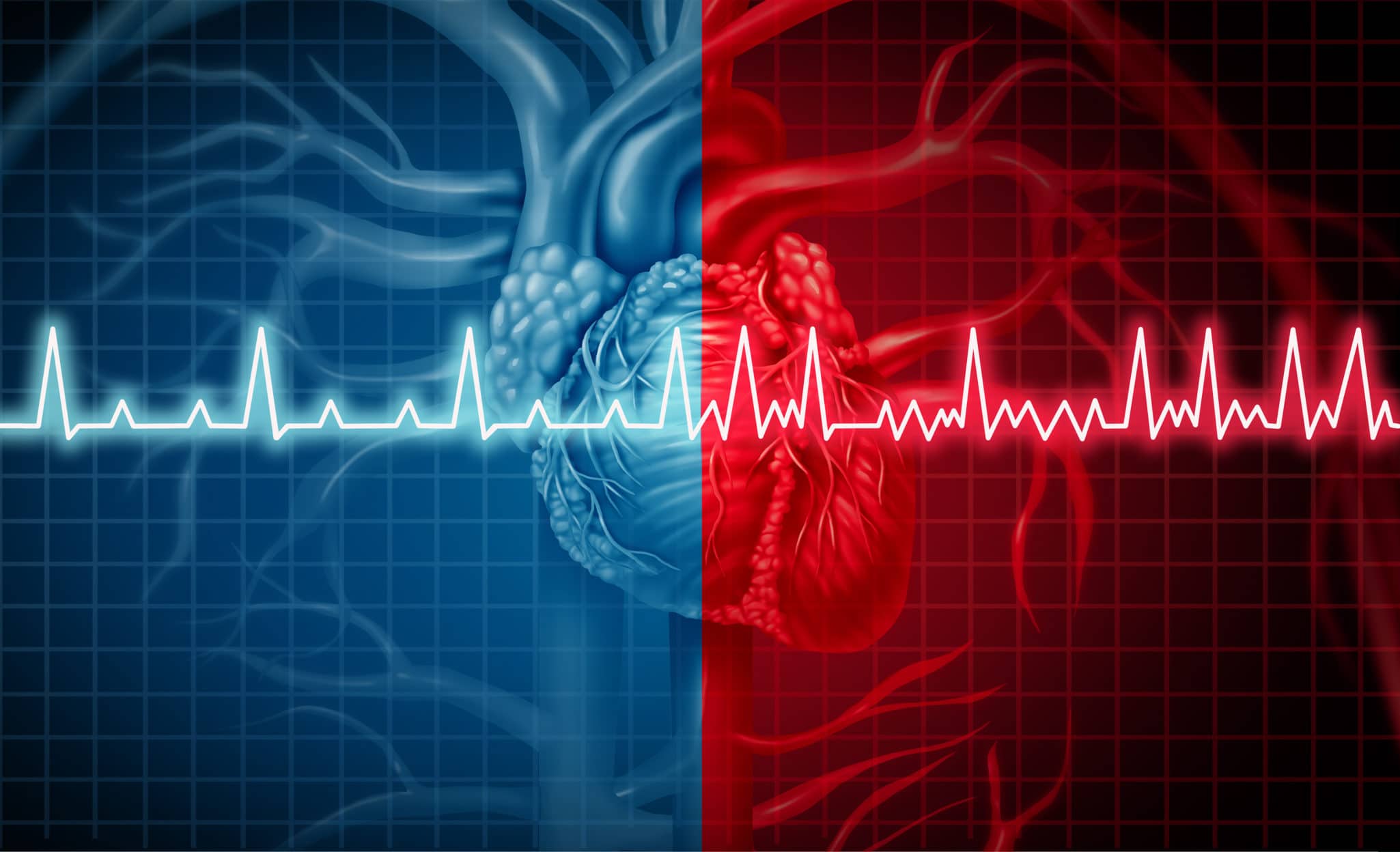
Atrial fibrillation, often referred to as "AFib", is an irregular heartbeat, a rapid heartbeat, or a quivering of the upper chambers of the heart, called the atria. Atrial fibrillation is due to a malfunction in the heart's electrical system and is the most common heart irregularity or cardiac arrhythmia. If you suffer from Atrial Fibrillation, Dr. Macy Smith offers a variety of treatment options to his patients in Birmingham, Alabama.
What Dr. Smith’s AFib patient’s say
"I am an 82 year old male who has been plagued with A-Fib for the last 12 years. Dr. Macy Smith was an answer to my prayers when he was hired by CVA. He has cared for my A-Fib for the last 5 years including 2 ablations and 1 Electrical Cardioversion and an excellent drug management program for me. He is kind, patient and a very caring person."
"I had been suffering from frequent atrial fibrillation for 13 years. Medications did not help and I was told by several cardiologists that there was nothing they could do and not to worry about it. On my first visit to Dr. Smith, he assured me that there was a remedy. Three weeks later he did a cardiac ablation. I had one more episode 2 weeks later but have had no other problems. I have my energy back and a renewed zest for life! Thank you Dr. Smith!!!"
Symptoms of AFib
Symptoms of atrial fibrillation may vary, depending on the patient. The most common symptom of AFib is a quivering or fluttering heartbeat. Some people have no symptoms and are unaware of their condition. The abnormal firing of electrical impulses in the heart causes the atria (the top chambers of the heart) to quiver. The clinical term for this is fibrillation, hence the name of the condition. There are other symptoms that point to a person having AFib:
- General fatigue
- Rapid or irregular heartbeat
- Fluttering or thumping in the chest
- Dizziness
- Shortness of breath
- Anxiety
- Faintness
- Confusion
- Fatigue when exercising
- Sweating
- Chest pain or pressure
The first time experiencing these symptoms, it may be really scary, and you may wonder, “Is this a heart attack?” After fibrillation stops, you may feel drained. For some people, AFib doesn’t stop and may continue on for hours, days, weeks, months, or even years. If you experience any of these symptoms, it is important to contact your doctor.
What causes Atrial Fibrillation?
When a person has AFib, their heart rate may range from 100 to 175 beats per minute, where a normal range is 60 to 100 beats per minute. Abnormalities or damage to the heart structure are behind most cases of atrial fibrillation. This is a list of possible causes:
- Heart attack
- High blood pressure
- Coronary artery disease
- Abnormal heart valves
- Congenital heart defects
- Overactive thyroid
- Stimulants such as medications, caffeine, tobacco
- Sick sinus syndrome (the improper function of the heart’s natural pacemaker)
- Lung disease
- Viral infection
- Previous heart surgery
- Stress from pneumonia or other illness
- Sleep apnea
Dr. Macy Smith Talks Atrial Fibrillation
Risk Factors for AFib
There are certain risk factors that make it more likely you may develop atrial fibrillation:
- Age — Older people are more likely to develop AFib.
- Heart disease — Any issues with the heart, such as coronary artery disease, increase your risk of AFib.
- High blood pressure — High blood pressure, if left unattended, can lead to AFib.
- Alcohol — Sometimes, drinking alcohol can trigger atrial fibrillation.
- Obesity
- Genetics
- Other chronic conditions — People with thyroid problems, sleep apnea, metabolic syndrome, diabetes, chronic kidney disease, and lung disease are at increased risk.
Types of Atrial Fibrillation (AFib)
The duration of a patient’s AFib makes for different classifications of the condition.
- Paroxysmal fibrillation — The heart returns to a normal rhythm on its own, or with intervention, within 7 days of the start of the episode. People with paroxysmal AFib may have episodes only a few times a year or may have more frequent symptoms.
- Persistent AFib — This is an irregular rhythm that lasts longer than 7 days. In this type of AFib, the heart will not return to its normal rhythm on its own.
- Long-standing AFib — The heart is consistently in an irregular rhythm for more than one year.
- Permanent AFib — The condition last indefinitely, and attempts to correct the rhythm have ended.
- Nonvalvular AFib — This AFib is not caused by a heart valve issue.
How serious is Atrial Fibrillation?
While atrial fibrillation may not sound serious and is often considered to be a minor health issue, it can actually be quite risky and potentially even life-threatening. Since the blood doesn’t properly move from the atria into the ventricles and then on to the rest of the body, it can starve the body of oxygen-rich blood, leaving you feeling weak, tired, or even incapacitated.
Atrial fibrillation can lead to serious complications:
- Stroke — Because the chaotic rhythm of the heart can allow blood to pool in the heart’s upper chambers, clots can form. If a clot forms and then dislodges, it can travel to the brain, block blood flow, and cause a stroke.
- Heart failure — Chronic AFib can weaken the heart and lead to heart failure.
Understanding Atrial Fibrillation
Prevention Strategies for AFib
To prevent atrial fibrillation from developing, a patient needs to follow the same protocols as to protect against a heart attack. A heart-healthy lifestyle involves these criteria:
- Staying physically active
- Eating a heart-healthy diet
- Not smoking
- Staying within a healthy weight
- Limiting alcohol and caffeine
- Reducing stress

Atrial Fibrillation Treatment
After Dr. Macy Smith diagnoses your atrial fibrillation with tests, such as electrocardiograms, echocardiograms, blood tests, stress tests, and even x-rays, he will design a treatment plan that will depend on certain facets of your condition. How long have you had AFib? How bothersome is it to you? And what are the underlying causes? The goal with treatment is to reset the rhythm or control the rate and to prevent blood clots and possible stroke.
Dr. Smith uses medications, nonsurgical procedures, surgical procedures, or a combination for treating AFib.
Medications
Medications have two purposes: to prevent and treat blood clots and to control heart rate and rhythm. The problem with the prolonged use of medication is possible side effects.
Non-Surgical Treatment
- Electrical cardioversion — This is a procedure where Dr. Smith administers an electrical shock to the outside of the chest using either paddles or patches. The shock can reset the heart’s normal rhythm.
- Catheter ablation — If medication and cardioversion aren’t successful in controlling the atrial fibrillation, catheter ablation may be used. This procedure destroys the area of the heart tissue that’s causing the erratic electrical signals, restoring your heart’s normal rhythm. A catheter is inserted into the groin blood vessel and is guided to the heart. There the catheter tip can deliver heat, cold, or radiofrequency energy to destroy “hot spots” on the heat where the erratic signals are originating.
- Convergent Therapy - Convergent therapy is a relatively new method for treating persistent Afib. It is a multidisciplinary, closed chest, minimally-invasive endoscopic procedure that uses ablation to create scar lines on the heart (both inside and outside) to return it to normal rhythm.
Surgical Treatment for AFib
- Surgical maze procedure — Conducted during open-heart surgery, a scalpel is used to create several precise incisions in the upper chambers of the heart. The goal is to create scar tissue because it can’t carry electrical signals, so it interrupts the erratic messages being sent with AFib.
- Pacemaker implantation — A pacemaker is a small electrical device implanted in the body near the collarbone. The device connects with wires attached to the heart. The pacemaker sends out an electrical signal to keep a steady contracting rhythm in the heart. It can also sense when the heartbeat becomes too fast or slow, and send signals to get the rate back in the normal range.
- WATCHMAN Implant — This is a one-time implantation procedure which reduces the risk of stroke originating in the Left Atrial Appendage (LAA). This is the source of blood clots from atrial fibrillation. The implant eliminates the need for blood thinners and for those at high risk of stroke from AFib.
How common is Atrial Fibrillation?
As we age, the incidence of atrial fibrillation increases. As Baby Boomers continue to age, we can expect to see the atrial fibrillation epidemic worsen. Today AFib impacts more than 5.1 million people in the United States, with expectations of 15.9 million by 2050.
These numbers, from the Mayo Clinic, only reflect those with atrial fibrillation confirmed by an electrocardiogram, and don’t include many more with symptoms but who cannot be confirmed. There are possibly also many more who don’t yet know they have it. The increase in obesity and stress in our society can be expected to accelerate the incidence of atrial fibrillation as well.
Schedule a Consultation with Dr. Macy Smith
If you suffer from Atrial Fibrillation (AFib) in Birmingham, AL, contact Dr. Macy Smith. Call 205-971-7566 to schedule a consultation to discuss your treatment options. Macy C. Smith, Jr. MD, FACC, FHRS treats Atrial Fibrillation and other heart disorders in Birmingham, Alabama and surrounding areas.